Research
Speaking with doctors and reception staff.
We wanted to gauge what the most limiting challenges are and learn more about GPs’ and receptionists’ daily routines at the surgery.
Too many unnecessary calls, too many people ending up on the triage list.
Almost 20% of the appointments are unnecessary.
Self care provision is currently paper based and inconsistent.
There are many people who need reassurance.
if people say they have been to pharmacist, what can you do…
Reviewing existing research.
Using existing research was crucial to our work in getting to know the wider primary healthcare space as well as more thoroughly understanding the self-care landscape.
One third of people see a GP for a self-treatable condition every year even though people have a desire to self-care they lose confidence in self-treating. People generally believe they can treat minor conditions but they’re not sure about the duration.
We were particularly informed by the Department of Health and Social Care Reviews Facility paper, a systematic review of qualitative and quantitative research of self-care for minor ailments. Notable findings included:
- Anxiety and belief that the severity and duration are beyond normal
- Past experiences of being prescribed medicines for minor ailments seemed like a confirmation of the need for medical intervention in any future illness
- Lack of sufficient knowledge and skills to implement self-care
- Lack of attention to self-care

Survey of the public.
There is a significant body of research quantifying the problem of
GP use for minor conditions but we wanted to go deeper into why
people see GPs for minor ailments, and when and why people use
other sources of support.
We ran a survey to answer these questions, with 75 responses.
Patients go online mostly to understand how to treat the condition, but also for help diagnosing. Government sources are a strong preference, valuing reliability.
The survey confirmed wider research studies of GP use, resorting to GPs in the belief their symptoms are going on for too long or it might be something more serious.
Many admitted they wanted reassurance. Only 20% of respondents were “ideal” self carers, and many don’t seek help. A few of these end up with more severe symptoms in part due to a lack of self-care.
Speaking with patients, the community and the general public
As well as speaking informally with people in the community we wanted to carry out deeper conversations with some of our survey respondents to understanding why they made particular self-care choices.
People don’t self-care consistently because they forget or it’s not convenient. People tend not to receive self-care advice from GPs and pharmacists and online information is a source of anxiety and greater GP use, not something that helped avoid it.
Research shows that people under 65 generally believe in being responsible with NHS resources, however it also shows a mismatch between this attitude and behavior. Many people don’t understand the term self-care. This creates a barrier between the health professionals and the patients.
Experience Mapping
Mapping the patient journey in the GP surgery helped us get to know all the touchpoints, as well as the challenges and emotional experience. Both online and offline interactions from prior to an appointment all the way through to post appointment were mapped giving us a foundation to identify opportunities.
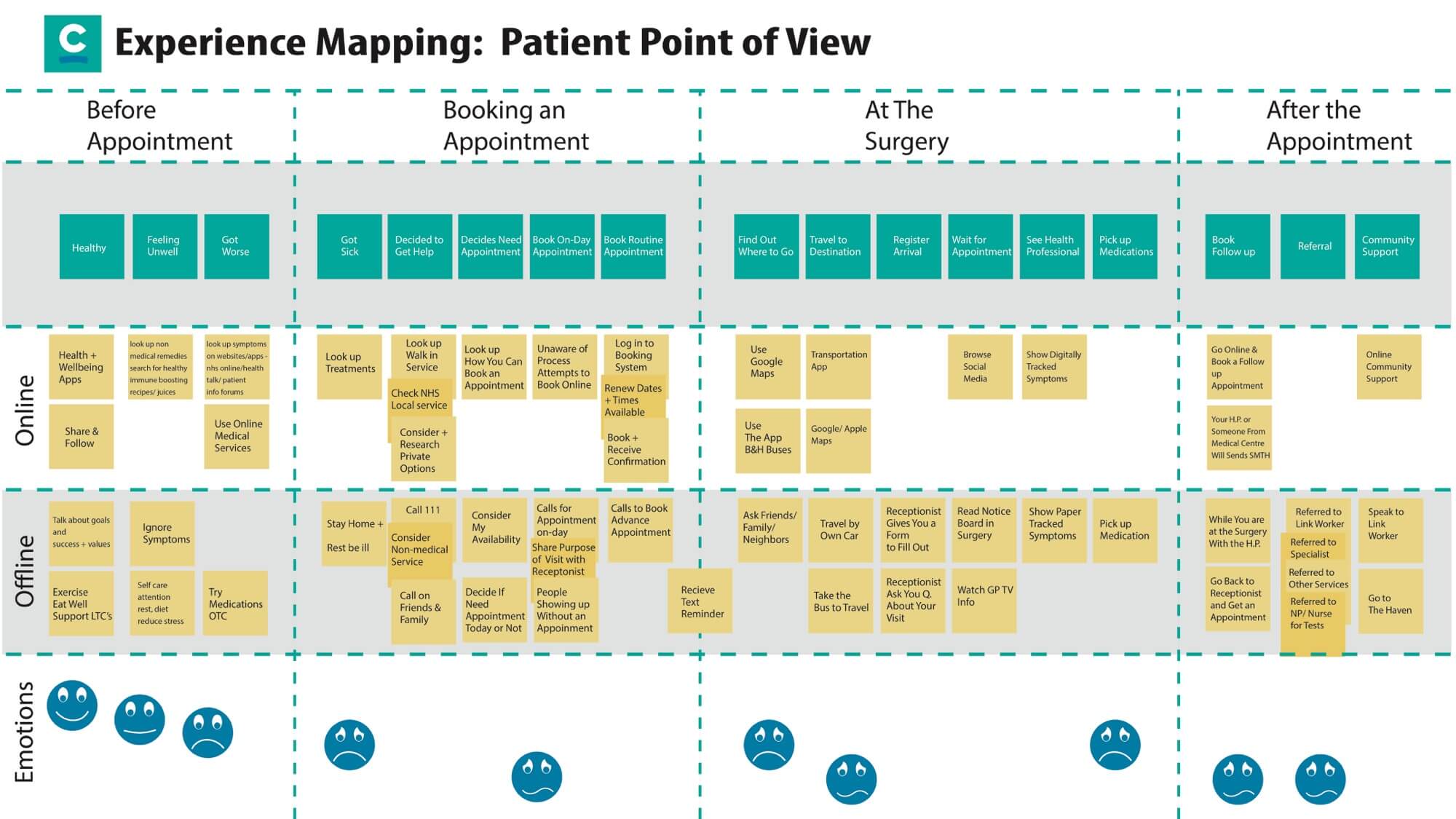
Design
Ideation
Design studios
This sketching session with Clearleft allowed for the collective pool of ideas to be turned on their head, combined, and moulded into new forms.
Having completed this we aggregated all the fantastic ideas and whittled these down to the most exciting concepts. We ran design studios at Henfield Medical centre with reception staff, nurses, and GPs. We started with warm-up sketching exercises to make everyone feel comfortable with sketching, and to help them start thinking outside the box.
We then planned to do a sketching session, which instead turned into a useful conversation around concepts.
Concept clarification
We developed five different problem areas, broad solution areas and concept summaries to assess and make decisions on focus.
A workshop with Clearleft helped us with valuable feedback and insight in terms of opportunity, project feasibility, development and scalability.
Using this feedback and discussions with Dr Sheppard we aggregated self-prescription and integrated self-care into a single concept to start designing.

Storyboarding
As we analysed the research findings, personas formed of shared characteristics, behaviors and beliefs towards the NHS. Using the three patient personas - Proactive, Worried Well and Stoic - we sketched their journeys when unwell, and interaction with services, to build empathy and really understand their needs.
After storyboarding, using different coloured flash cards for our respective personas we started to see the opportunity areas within the user journey and quickly generated ideas for each opportunity.

Final concept
At this point we started to see the connection between the more compelling ‘mini-ideas’ and the formation of a user journey that addresses a range of problems and opportunities for our different personas. From a user journey we moved into basic wireflows.
Discussions with developers helped clarify technical constraints and options for delivery. We were also aware that we didn’t want to create barriers to the solution by introducting the requirement to download a native app. As a result we decided on a progressive web app to deliver the digital element of the service.

Prototyping
Interfaces
As we developed the content we created high fidelity screens of the key interfaces. This was made easier with the use of the NHS Digital Service Manual, the NHS’s digital design system, as we wanted to use familiar, trusted visual language. A combination of Invision and Flinto helped us create clickable prototypes and animation of screens for the film.
Testing
We used guerrilla concept testing to understand how people interacted with the pharmacy card, a key part of the Self Treat service. Using a scenario we were able to get feedback on how the card was received and what people would expect to see when scanning the QR code.
Time constraints meant our testing was limited. Should this concept be developed further we would envision further concept testing with a fully designed pharmacy card, followed by usability testing of the interfaces and communications.

Communication
Deciding on the outcome
Due to the scale and complex nature of our concept and limited time we had left we decided to make a film to communicate the vision of the project.
Storyboarding the film
Aware that the result of the project was a high level vision we knew that telling the story of how things are now, and how they could be, was crucial to communicating the value. Sketching the flow of scenes needed to share this idea was invaluable, and gave us the base from which to add text to aid our storytelling. It also helped us develop only the necessary prototype screens needed in the film.
Shooting and editing
Shooting all the scenes in different locations in one day was one of the biggest challenges we faced during this internship. However, the shooting day went smoothly as we carefully and meticulously planned all logistics to ensure we were fully prepared for the shoot.
We only had one day for the complete editing of our video, so likewise we gathered everything we might have needed prior to this day to successfully speed up the process.

